Hemorrhoids are a common and uncomfortable condition affecting millions of people worldwide. Understanding hemorrhoids meaning, recognizing hemorrhoids symptoms, and knowing available hemorrhoids treatment options can help you find relief and prevent future occurrences.
What Are Hemorrhoids? Understanding Hemorrhoids Meaning
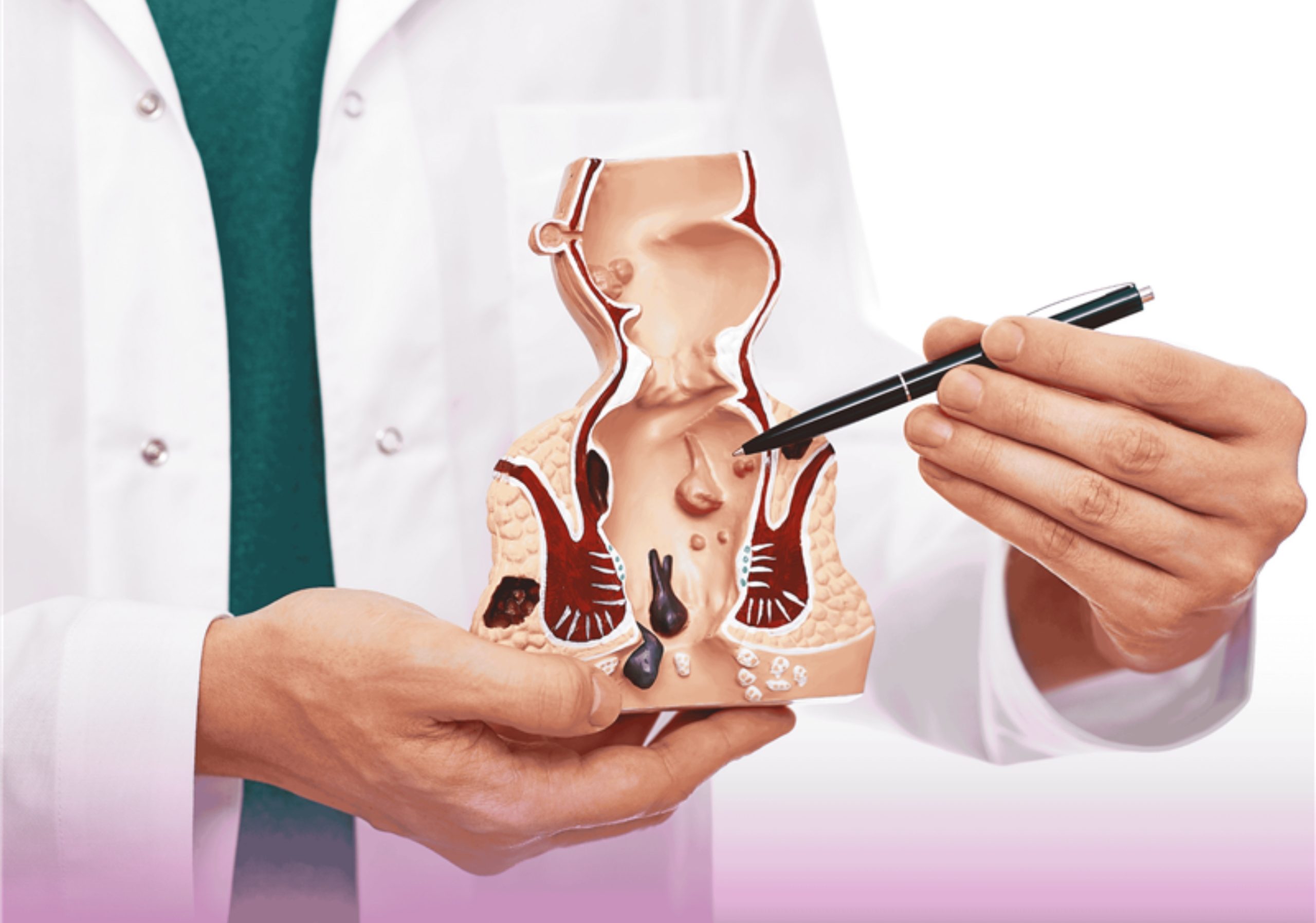
Hemorrhoids are swollen blood vessels in the rectum or anus that develop due to increased pressure in the lower rectum. These enlarged veins cause discomfort, pain, and irritation, significantly impacting daily life quality.
Hemorrhoids are classified into two main types:
Internal Hemorrhoids – Located inside the rectum, usually painless but may cause bleeding during bowel movements.
External Hemorrhoids – Found under the skin around the anus, causing pain, swelling, and intense itching.
A thrombosed hemorrhoid occurs when a blood clot forms inside an external hemorrhoid, causing severe pain and significant swelling.
Common Hemorrhoids Symptoms to Watch For
Recognizing hemorrhoids symptoms early helps ensure prompt treatment. Key symptoms include:
- Rectal bleeding – Bright red blood on toilet paper or in stool
- Anal itching and irritation – Persistent discomfort around the anus
- Pain during sitting – Especially noticeable during prolonged sitting
- Visible swelling or lumps – Particularly noticeable with external hemorrhoids
- Mucus discharge – Clear or colored discharge from the anus
- Feeling of incomplete evacuation – Sensation that bowel movements are incomplete
External hemorrhoids symptoms specifically include visible lumps around the anus, severe itching, and sharp pain that worsens when sitting or during bowel movements.
What Causes Hemorrhoids?
Several factors contribute to hemorrhoid development:
- Chronic constipation or diarrhea
- Straining during bowel movements
- Prolonged sitting, especially on the toilet
- Pregnancy (increased pressure on pelvic veins)
- Low-fiber diet leading to hard stools
- Obesity and excess weight
- Heavy lifting or frequent straining
- Aging and weakened tissue support
Comprehensive Hemorrhoids Treatment Options
1. Home Remedies for Hemorrhoids Treatment
Dietary Modifications:
- Increase fiber intake through fruits, vegetables, and whole grains
- Drink plenty of water to soften stools
- Avoid spicy foods and alcohol that may worsen symptoms
Lifestyle Changes:
- Take warm sitz baths for 10-15 minutes several times daily
- Apply cold compresses to reduce swelling
- Use over-the-counter topical treatments with hydrocortisone
- Avoid prolonged sitting and straining during bowel movements
2. External Hemorrhoid Treatment Options
External hemorrhoids require targeted treatment approaches:
Topical Treatments:
- Witch hazel pads for cooling relief
- Hemorrhoid creams containing lidocaine for pain relief
- Anti-inflammatory medications to reduce swelling
Professional External Hemorrhoid Treatment:
- Rubber band ligation for protruding hemorrhoids
- Sclerotherapy injections to shrink hemorrhoids
- Infrared coagulation for tissue reduction
3. Advanced Hemorrhoids Treatment Procedures
Conventional Hemorrhoidectomy (Milligan-Morgan or Ferguson Technique)
- Gold standard for Grade III-IV hemorrhoids
- Provides definitive treatment with excellent long-term results
- Requires careful post-operative pain management
Hemorrhoidal Artery Ligation (THD)
- Minimally invasive techniques using Doppler ultrasonography
- Lower recurrence rates with reduced post-operative discomfort
- Ideal for internal hemorrhoids with minimal external prolapse
External Thrombectomy
- Indicated for acute thrombosed external hemorrhoids
- Must be performed within 72 hours of symptom onset
- Provides immediate pain relief and prevents prolonged recovery
Laser Hemorrhoidoplasty (LHP)
- Utilizes focused laser energy to shrink hemorrhoidal tissue
- Most effective for Grade II and III hemorrhoids
- Preserves surrounding healthy tissue while treating affected areas
Post-Treatment Care and Recovery
Proper post-treatment care ensures optimal healing:
Pain Management:
- NSAIDs for inflammation control
- Topical lidocaine for localized pain relief
- Prescription pain medication if necessary
Wound Care:
- Regular sitz baths to promote healing
- Fiber supplementation to prevent straining
- Stool softeners to maintain comfortable bowel movements
Follow-Up Care:
- Monitor for complications like bleeding or infection
- Schedule regular check-ups with healthcare provider
- Watch for signs of anal stenosis or recurrence
Preventing Hemorrhoids: Long-Term Strategies
Effective hemorrhoid prevention includes:
- Maintaining a high-fiber diet with adequate hydration
- Regular exercise to prevent constipation
- Responding promptly to bowel movement urges
- Avoiding prolonged sitting periods
- Managing weight to reduce pelvic pressure
- Practicing proper bathroom hygiene
When to Seek Professional Hemorrhoids Treatment
Consult a healthcare provider immediately if you experience:
- Heavy or persistent rectal bleeding
- Severe pain or significant swelling around the anus
- Symptoms that don’t improve with home treatment
- Signs of infection like fever or pus discharge
- Changes in bowel habits or stool appearance
Conclusion
Understanding hemorrhoids symptoms and available hemorrhoids treatment options empowers you to seek appropriate care. Whether dealing with external hemorrhoids or internal varieties, effective treatments range from simple home remedies to advanced surgical procedures. Early intervention and proper external hemorrhoid treatment can prevent complications and improve quality of life.
For persistent symptoms or concerns about the effectiveness of hemorrhoids treatment, consider consulting one of the top general surgeons to receive expert medical advice and tailored treatment recommendations.