Esophageal cancer surgery is among the most complex operations in gastrointestinal surgery. Traditionally requiring large incisions, prolonged hospital stays, and lengthy recovery periods, it’s a procedure many patients fear. But advanced minimally invasive techniques are changing that narrative. A 73-year-old patient recently underwent a groundbreaking laparoscopic-thoracoscopic Ivor Lewis esophagectomy at Burjeel Hospital, Abu Dhabi, and was discharged just four days later—a testament to surgical innovation and expertise.
The Patient’s Journey
For three years, the patient suffered from gastroesophageal reflux symptoms that responded to PPI therapy. However, he recently developed dysphagia (difficulty swallowing solids), prompting further investigation.
Medical history included:
- Long-segment Barrett’s esophagus under surveillance
- Hyperlipidemia
- Hypertension
- Coronary artery disease (3 coronary stents, dual antiplatelet therapy)
- Non-smoker
Endoscopy revealed what surveillance was designed to detect: a biopsy-proven moderately differentiated adenocarcinoma of the distal esophagus.
Comprehensive Staging
CT Scan findings:
- Long-segment asymmetric circumferential wall thickening (9mm)
- Involving distal 6.7cm of esophagus
- Mild luminal narrowing with proximal dilatation
- No evidence of metastatic disease
PET Scan results:
- FDG-avid (SUV 4.36) hypermetabolic wall thickening
- Few hypermetabolic hilar and paratracheal lymph nodes (SUV 2.5-3.0)
- No distant organ deposits
Endoscopic Ultrasound (EUS): Dr. Khalid Elsayed, Consultant Gastroenterologist, performed EUS showing a superficial esophageal malignant nodule at 35cm, which he removed using endoscopic submucosal dissection (ESD) technique.
Histopathology revealed: Moderately differentiated adenocarcinoma, at least stage pT1b with positive deep resection margin.
The Oncology MDT Decision
Given the incomplete ESD and cancer stage of at least pT1b (carrying up to 20% risk of lymph node metastases), the Multidisciplinary Team decided to offer esophagectomy for complete cancer removal.
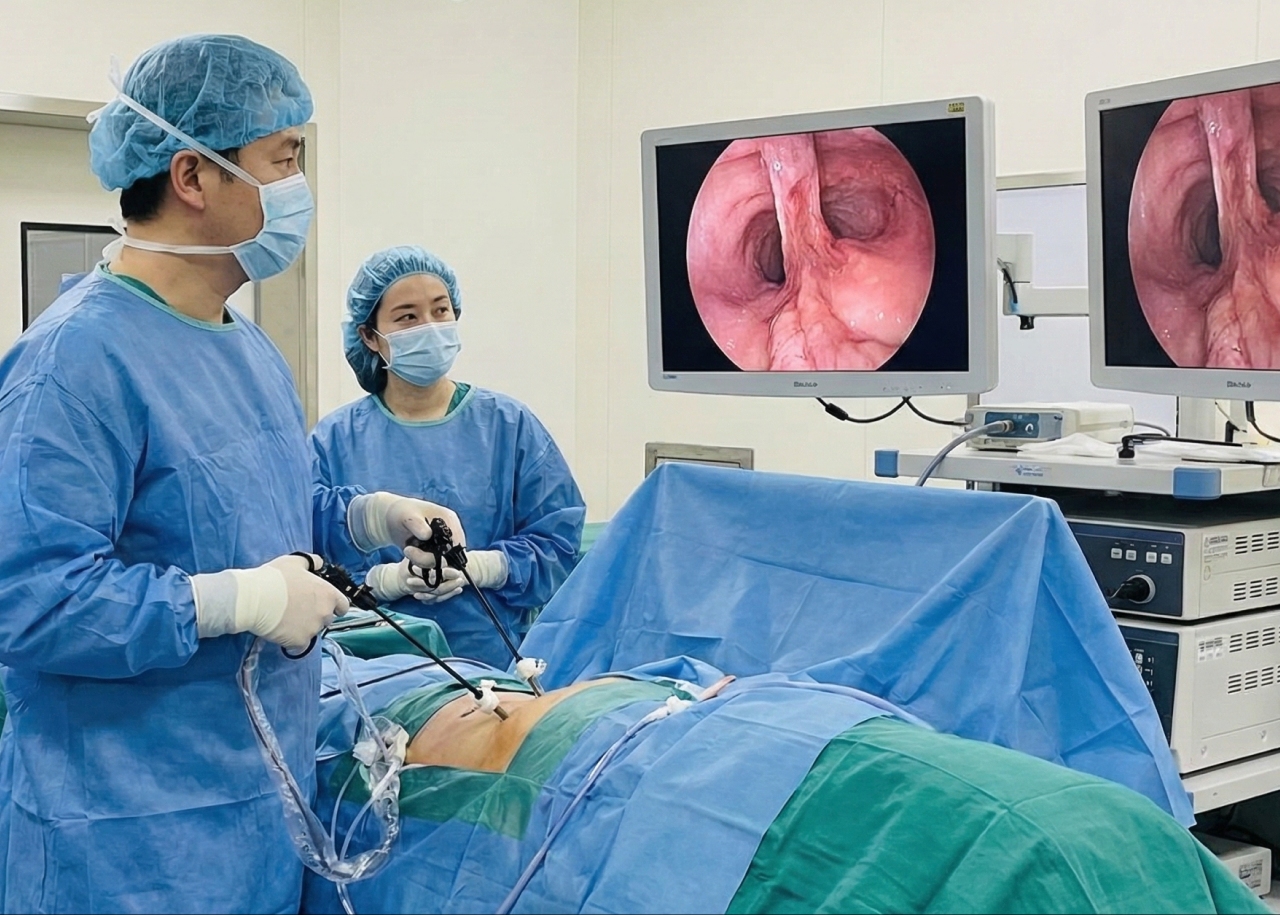
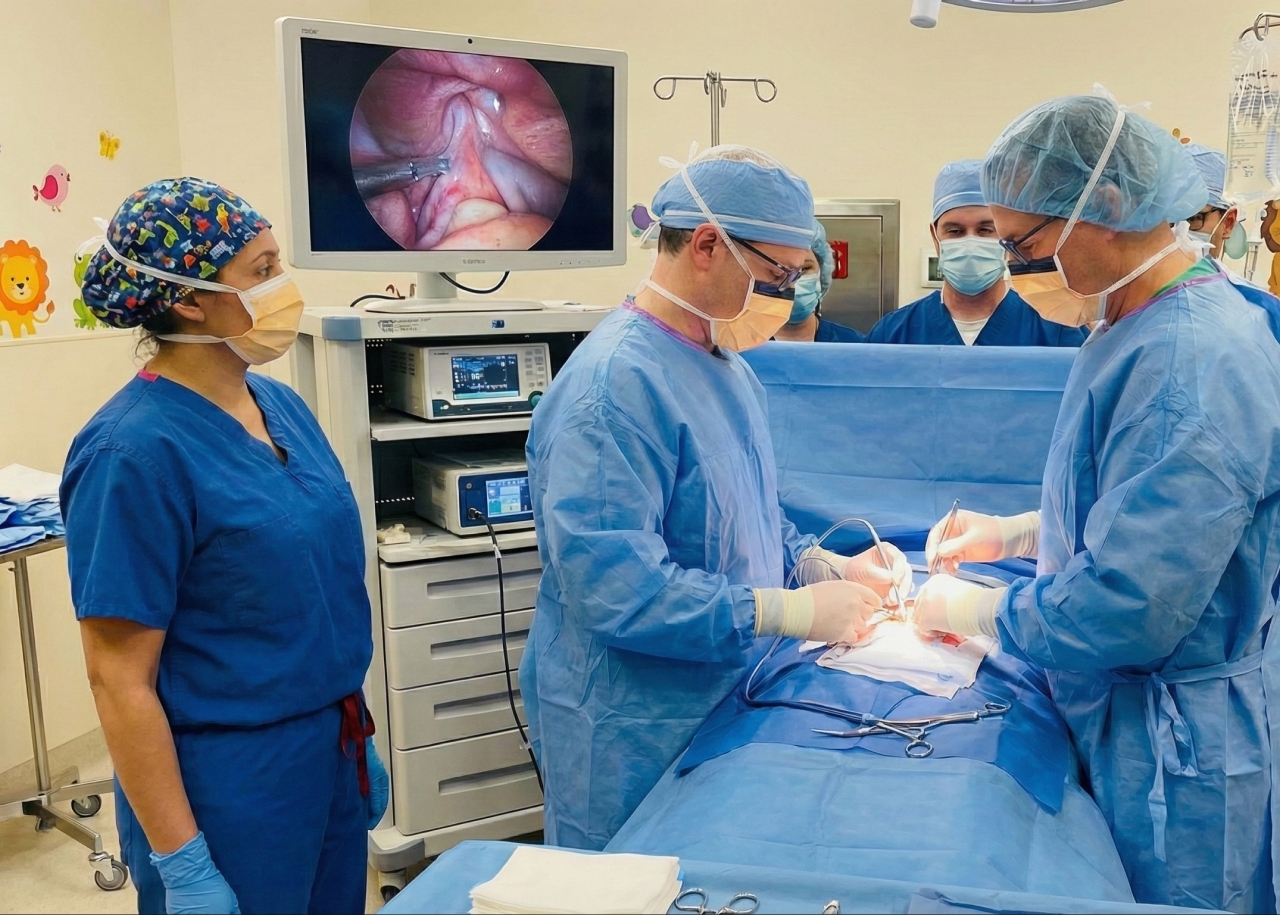
The Minimally Invasive Approach
The patient underwent laparoscopic-thoracoscopic Ivor Lewis cardio-esophagectomy with D2 lymphadenectomy and pyloroplasty.
Why this matters: Most centers perform this operation through large open incisions. The minimally invasive approach offers:
- Smaller incisions
- Less post-operative pain
- Faster recovery
- Shorter hospital stay
- Better cosmetic outcome
- Reduced complications
The Five-Hour Surgical Journey
Stage 1: Abdominal Phase (Lloyd Davis Position)
- Proximal gastrectomy en bloc with regional lymphadenectomy
- Construction of gastric tube
- Pyloroplasty
- Laparoscopic approach throughout
Stage 2: Thoracoscopic Phase (Prone Position, Single Lung Ventilation)
- Esophagectomy completed by dividing mid-esophagus with stapler
- Regional lymphadenectomy performed
- Gastric tube pulled into chest (avoiding twisting)
- Thoracoscopically-sutured end-to-side esophago-gastric anastomosis
- Methylene blue leak test: negative
- Specimen placed in water-impervious bag and pushed through hiatus into abdomen
Stage 3: Final Abdominal Phase
- Hiatus closed (preventing visceral herniation into chest)
- Specimen retrieved through Pfannensteil incision (avoiding painful thoracotomy)
- Thoraco-abdominal drain placed
Blood loss: 50ml
Blood transfusions: None (intraoperative or postoperative)
Frozen Section Verification
During surgery, frozen sections of proximal and distal resection margins returned negative—confirming complete tumor removal with clear margins.
Remarkable Recovery
Postoperative Course:
- No complications
- Discharged on postoperative day 4
- On full liquid diet
- Remained well at 6-week follow-up
Traditional approach comparison:
- Open surgery typically requires 10-14 day hospital stay
- More pain and slower mobilization
- Larger incisions with extended healing time
Final Pathology Results
- Moderately differentiated esophageal adenocarcinoma
- Stage: pT1bN0
- All 32 lymph nodes: negative for metastases
- Resection margins: negative (R0 resection—complete removal)
Oncology Follow-up Management
The Oncology MDT reviewed the final pathology and determined: Follow-up only (no adjuvant chemoradiotherapy required).
This excellent outcome reflects:
- Early detection through surveillance
- Complete surgical removal
- No lymph node involvement
- Clear margins
Understanding Barrett’s Esophagus and Cancer Risk
Barrett’s esophagus is a condition where chronic acid reflux changes the lining of the esophagus. While most people with Barrett’s never develop cancer, regular surveillance is crucial because:
- Small percentage progress to cancer
- Early detection significantly improves outcomes
- Minimally invasive treatment options available for early-stage disease
- Cure rates are high when caught early
The Surgical Excellence Behind This Success
This case demonstrates several aspects of advanced surgical care:
- Minimally Invasive Expertise: Few surgeons worldwide perform this complex operation laparoscopically
- Multidisciplinary Collaboration: Gastroenterology, surgery, oncology, pathology, and anesthesia working seamlessly
- Advanced Techniques: Thoracoscopic anastomosis construction, Pfannensteil retrieval avoiding thoracotomy pain
- Patient-Centered Care: Balancing cancer cure with quality of life and recovery
Why Choose Burjeel for Esophageal Cancer
- Minimally invasive esophageal surgery expertise
- Multidisciplinary tumor board
- Advanced endoscopic techniques (ESD, EUS)
- Intraoperative frozen section capability
- Comprehensive oncology services
- Enhanced recovery protocols (ERAS)
- Shorter hospital stays
- Better outcomes
Our Experts

Prof. Dr. Basil Ammori
Consultant – Laparoscopic Bariatric, Gastrointestinal, Hepatobiliary and Pancreatic Surgeon
Burjeel Hospital, Abu Dhabi
Advanced Gastrointestinal Cancer Care
Esophageal cancer requires specialized expertise and a multidisciplinary approach. Our team provides comprehensive evaluation, advanced surgical options, and ongoing oncology support.
For Appointments & Consultations: